Should you pop a blister? How can you speed up healing?
When and how should you pop a blister? And how can you speed up the healing? The only reason to pop a blister is to prevent it spreading, otherwise leave it alone. Naturally, it's better to prevent the blister in the first place.
Contents
1 Don't Pop the Blister
The only reason to pop a blister is when pressure will cause the blister to spread; if the blister is not going to spread due to pressure, leave it alone. A wound heals faster in a moist environment than when dried out[1]. Likewise, popping a blister is a bad idea as a blister will heal faster and better when left intact. The idea of 'drying out' a wound is dated and wrong. Drying out a wound or bursting a blister can also increase the scar tissue that is left behind. The fluid inside a blister creates a good healing environment, far better than any dressing. The biggest problem with popping a blister is it introduces the possibility of infection. To make matters worse, a popped blister may refill with fluid, which is the worst of both worlds. Typically popping a blister will also make things more painful, so don't pop to reduce your discomfort. The fluid acts as a cushion to protect the raw flesh under the blister, so once the blister is popped, the two surfaces will then rub.
1.1 Moleskin Doughnut
The alternative to popping a blister due to pressure is to build up the area around the blister so that the pressure is relieved. Moleskin can be cut out in the shape of the blister, forming a doughnut shape that reduces pressure on the blister if it is small enough.
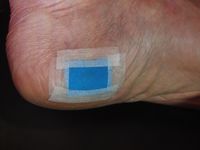
1.2 Taping Blisters
Putting tape over a blister on your foot can help reduce the pain. Care must be taken to ensure the tape does not peel up, causing further blistering. See Taping for more details.
2 How to Pop a Blister
If you have to pop a blister, your biggest risk is from infection. Bursting the blister will impair healing, but an infection will obviously make things far worse. Follow these steps...
- Clean your hands to make sure they are sterile.
- Sterilize the area first by wiping with an antiseptic wipe. Make sure you wipe the whole blister and the surrounding area.
- Ideally you should have a sterile tool to burst the blister. If you are using scissors, or anything else that is not in a sterile package, you must sterilize it. I use hypodermic needles for bursting blisters as they are very sharp and quite long. (One caution: hypodermic needles can be considered 'drug paraphernalia' if you don't have a good medial reason for having them.)
- Puncture the blister at the edge, ideally at the edge that will be lowest most of the time so that gravity aids drainage. Multiple punctures may be needed to provide sufficient drainage.
- Use a sterile dressing to push out the fluid, taking time to ensure you remove as much as possible. You can use an antiseptic wipe for this, but getting any of the antiseptic into the blister can be quite painful.
- Cover the blister with a dressing. An occlusive (waterproof) dressing will improve healing and reduce the chance of infection[2].
- Ideally, use a 'hydrocolloid' dressing, such as Band-aid Advanced Healing Blister Cushions. A hydrocolloid dressing is one that is water and air tight, with a gel that absorbs fluids. This can keep the wound moist without becoming saturated (macerated).
- You may need an adhesive promoter such as tincture of benzoin to help keep things in place. Be careful with tincture of benzoin: If you put it near the punctures in the blister it can seep inside and be remarkably painful.
- Putting an adhesive promoter on the blister itself will mean that the blister and the dressing are bonded. When you then try to remove the dressing, it will take the skin of the blister with it. If possible apply tincture of benzoin only to the surrounding skin.
- Putting a small amount of antibiotic ointment on the blister itself will help reduce the chance of infection. It will also stop the dressing sticking to the dead skin, but care must be taken to avoid spreading the ointment and preventing the dressing sticking.
- If possible, leave the blister alone. Do not change the dressing unless it starts to come off or leaks. You can leave the blister covered for up to a week.
- Do not let the blister dry out, but keep it moist to improve healing.
3 Other Techniques
There are two techniques I will mention, but would not recommend.
- Threading a strand of cotton through a blister will make it more likely to continue to drain. However, this will also increase the risk of infection, reducing the number of bacteria need to cause an infection by 10,000x[3].
- Injecting tincture of benzoin into the blister after it is emptied glues the detached skin to the underlying flesh. Alternatively the blister can be cut open to apply the tincture of benzoin. This was a common practice in the US army in the 1980s, and while effective in the short term it caused issues with fissures and some cases of infection, and the practice has been abandoned[4]. The pain from the tincture of benzoin is intense, and the overall pain of the blister is not necessarily lessened, but it may allow continued movement. A similar practice is to use superglue.
4 Speeding up healing
There are several ways of speeding up the healing process.
4.1 Apply Heat
Keeping the blister warm improves blood flow and healing. You can use a heating blanket like a Theratherm, but this requires power and is inconvenient. Instead, using chemical hand warmers will keep the blister area warm for hours. I like to use the larger sized 'hot hands' warmers which keep warm for over 12 hours so I can replace them twice a day. I've found the hand warmers will not get too hot but be careful as a burn will obviously not speed up healing! For foot blisters, placing the warmer inside a thick hiking sock works well.
4.2 Continuous Protein Intake
I have found that keeping a steady intake of protein speeds up the healing process. It's particularly important to take some protein before bed time, as a lot of healing occurs while you sleep. If the body does not have a supply of protein available, it can't make repairs. Check out GOMAD Grazing for my approach to continuous protein intake.
4.3 Omega-3
Main article: Omega 3
Omega-3 oils are important for wound healing[5]. I take both Flax Seed Oil and Fish Oil. I blend the Flax Seed Oil into a protein shake, but the fish oil I take tastes great on it's own.
4.4 Calorie Intake
It's important to keep your calorie intake adequate. If you are dieting, then your body will slow down the healing process to conserve energy.
4.5 Avoid NSAIDs
Main article: NSAIDs and Running
Ibuprofen, and possibly other NSAIDs, impair wound healing and should be avoided[6][5]. (Tobacco usage also causes wound healing problems[6].)
4.6 Take Vitamins
A number of vitamins and minerals are needed for wound healing, including[6]:
- Vitamin C
- Iron
- Vitamin A
- Zinc
- Copper
- Calcium
Of these, Vitamin C is arguably the most critical for wound healing. In addition, Vitamin E may improve the strength of the wound and deficiencies in B vitamins may impair the immune system. Getting these nutrients from wholesome foods is ideal, but supplementation may be appropriate.
4.7 Reduce Stress
Studies have shown that stress will delay wound healing[5] so reduce stress if possible.
4.8 Bioelectric Wound Dressings
There are some studies that have shown that a Bioelectric wound dressing improves healing[7], with one study showing a 36% improvement in healing time compared with a semi-occlusive dressing[8]. These Bioelectric wound dressings are not externally powered, but use embedded 'microcell batteries'. One provider is http://www.procellera.com/, but the dressings are not readily available and are expensive. (The use of electrical stimulation for healing wounds that do not respond to other treatments has been shown effective and is medically approved[9], but that is outside of the scope of this article.)
5 Blister Color
The contents of the blister is normally a yellowish clear liquid, blood or pus[10]. The clear, yellowish fluid is called serous and is similar to blood plasma. The difference between serous and blood is that the latter means that some capillaries are damaged under the blister. The presence or absence of blood does not appear to be medically significant. If the blister is filled with pus, this may indicate an infection, but this is not always the case.
6 References
- ↑ Charles K. Field, Morris D. Kerstein, Overview of wound healing in a moist environment, The American Journal of Surgery, volume 167, issue 1, 1994, pages S2–S6, ISSN 00029610, doi 10.1016/0002-9610(94)90002-7
- ↑ WH. Eaglstein, Moist wound healing with occlusive dressings: a clinical focus., Dermatol Surg, volume 27, issue 2, pages 175-81, Feb 2001, PMID 11207694
- ↑ SD. ELEK, Experimental staphylococcal infections in the skin of man., Ann N Y Acad Sci, volume 65, issue 3, pages 85-90, Aug 1956, PMID 13363202
- ↑ Personal email communication with Army medic.
- ↑ 5.0 5.1 5.2 S. Guo, L. A. DiPietro, Factors Affecting Wound Healing, Journal of Dental Research, volume 89, issue 3, 2010, pages 219–229, ISSN 0022-0345, doi 10.1177/0022034509359125
- ↑ 6.0 6.1 6.2 Wayne K. Stadelmann, Alexander G. Digenis, Gordon R. Tobin, Impediments to wound healing, The American Journal of Surgery, volume 176, issue 2, 1998, pages 39S–47S, ISSN 00029610, doi 10.1016/S0002-9610(98)00184-6
- ↑ Assessment of the effects on wound healing and gene expression of a bioelectric dressing using a porcine wound model and real time reverse transcriptase-polymerase chain reaction, Journal of the American Academy of Dermatology, volume 60, issue 3, 2009, pages AB200, ISSN 01909622, doi 10.1016/j.jaad.2008.11.868
- ↑ Andrew Blount, Sarah Foster, Richard Wilcox, Use of Bioelectric Dressings for Faster Wound Healing: A Prospective Case Series, Plastic and Reconstructive Surgery, volume 126, 2010, pages 97, ISSN 0032-1052, doi 10.1097/01.prs.0000388820.96542.6e
- ↑ LC. Kloth, Electrical stimulation for wound healing: a review of evidence from in vitro studies, animal experiments, and clinical trials., Int J Low Extrem Wounds, volume 4, issue 1, pages 23-44, Mar 2005, doi 10.1177/1534734605275733, PMID 15860450
- ↑ Fitzpatrick's Dermatology in General Medicine, ISBN 0071669043

