Mortons Neuroma, symptoms and fixes
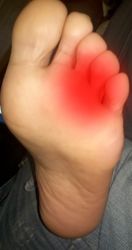
Morton's Neuroma is a common problem in runners, and there are a number of simple fixes you can try before resorting more drastic solutions like sclerosing or surgery. A Morton's Neuroma normally causes a burning pain in the forefoot, just behind the 3rd and 4th toes (sometimes behind the 2nd and 3rd toes). The pain often radiates towards the toes, and sometimes there is numbness rather than pain. The underlying cause is inflammation of the nerve between the bones of the forefoot, often triggered by narrow or tight shoes. I have had good results with the simple fixes described below, and I have had reports of other runners with similar success.
Contents
[hide]1 Causes of Morton's Neuroma
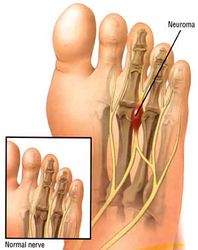
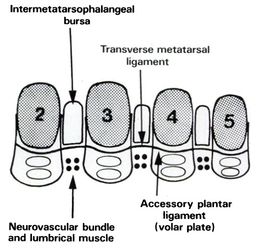
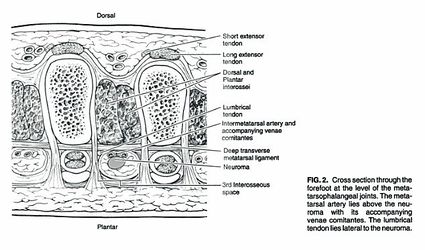
A Morton's Neuroma is not a true neuroma, which is a tumor that is generally benign. Rather, it is an enlargement of the nerve where it goes between the metatarsal bones of the foot. Because the nerve no longer fits between the gap, the pressure causes pain and sometimes numbness. This enlargement of the nerve is often an inflammation due to irritation. If the forefoot becomes compressed due to shoes that are too narrow, the nerve becomes damaged and inflamed. This inflammation means the nerve no longer fits in the space between the bones, creating further irritation and more inflammation. If this vicious circle can be broken, the problem may be resolved. However, in some situations the nerve can have fibrous tissues formed around it, which may require the destruction of the nerve or surgical removal.
2 Morton's Neuroma Symptoms
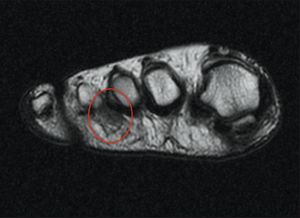
The classic symptoms of Morton's Neuroma are a pain on the lower (plantar) surface of the foot, located between the 3rd and 4th metatarsal heads, though it can happen less commonly between other metatarsal's. The picture below shows the location of the inflamed nerve. The pain can be dull or sharp, and is often burning, occasionally radiating to the toes. Sufferers often find that removing footwear or massaging the area helps relieve the pain.
3 Alternative Explanations (Differential Diagnosis)
There are other problems that can have similar symptoms to a Morton's Neuroma. The most likely problems are a stress fracture (or stress reaction) and intermetatarsal bursitis.
- A stress fracture in the metatarsal bones of the foot can produce similar pain to a Morton's Neuroma. Stress fractures are hard to diagnose, and won't generally show up on an x-ray. An MRI may reveal a stress fracture, but if the fracture is at the metatarsal head it can be overlooked as these are relatively rare.
- A stress reaction is the changes in the bone that occur with excessive stress, but before a fracture occurs. These stress reactions may show up as an edema-like bone marrow abnormality on an MRI.
- The bursitis is an inflammation of the small, fluid-filled sacs (bursae) that provide cushioning to the bones, tendons and muscles near joints. There are bursae between the metatarsals that can become inflamed and produce symptoms similar to Morton's Neuroma.
While rare, it's also possible for the symptoms to indicate a sesamoid fracture, nodules associated with rheumatoid arthritis, synovial cyst, soft tissue chondroma, and plantar fibromatosis. I talked to one runner who had symptoms of a Morton's Neuroma which turned out to be caused by large calluses under the forefoot.
4 Diagnosing Morton's Neuroma
Morton's Neuroma is not easy to diagnose clearly, but these are the primary tests.
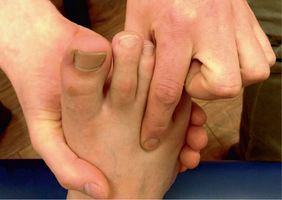
- Mulder's Test. While not the most accurate diagnosis, it's easy to perform. The test simply puts pressure on the neuroma to see if this elicits pain. One hand is used to squeeze the sides of the forefoot, pressing the metatarsal heads together, and the fingers of the other hand are used to squeeze the area between the metatarsal heads (where the pain is located). The pain is sometimes accompanied by a click the can be felt, called Mulder's click, further suggesting a Morton's neuroma.
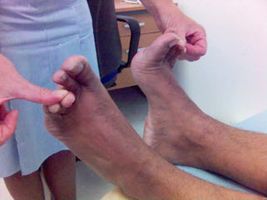
- Digital Nerve Stretch Test. While not as commonly used as Mulder's, this is another simple test. Both ankles are held in full dorsiflexion (toes pulled towards the shins), while the toes either side of the suspected Morton's Neuroma are manually extended on both feet (see picture below). Pain in the suspected location indicates a Morton's Neuroma.
- MRI. The best diagnostic tool is an MRI, where a Morton's Neuroma is indicated by a Neuroma of 5mm or more. The MRI should be performed in the prone position with the foot plantar-flexed (toes pointed) and without contrast enhancement. If the neuroma is smaller than 5mm then other conditions should be considered. On the other hand, a negative MRI result does not exclude the possibility of a Morton's Neuroma as studies have shown false negative rates of 17% and studies suggest that 30-35% of subjects have a Morton Neuroma without any symptoms.
- Ultrasound. Ultrasound can be used to diagnose Morton's Neuroma, but one study found that Ultrasound only found 56% of cases and there are concerns of a high false positive rate, so MRI is preferred. Ultrasound imaging is quite dependent on the technique and interpretation of the operator.
5 Fixing Morton's Neuroma
A Morton's neuroma can be a difficult thing to fix once it flares up. The longer the symptoms persist, the harder it can be to fix the problem, so don't ignore it. I recommend starting with conservative approaches before resorting to surgical intervention.
- Getting a clear diagnosis is important, as the treatment for a stress fracture and Morton's neuroma are quite different. Get an MRI from a practice that specializes in the foot problems of athletes and has extensive experience with Morton's neuroma.
- It's critical to prevent the nerve being aggravated further. Avoid any footwear that compresses the sides of your foot or is too narrow. Wearing the wrong shoes, even for a short period of time, can cause a Morton's neuroma to flare up for weeks. Changing footwear may help in over 40% of cases.
- I resorted to cutting away the sides of my shoes at the forefoot to prevent pressure aggravating my Morton's Neuroma. See below for details.
- I used the overnight toe spreading socks (see below) to help heal the Morton's Neuroma I had. This approach gently spreads the metatarsal heads to give the nerve room to recover and prevent irritation.
- Many people find that a metatarsal pad in their shoes help relieve the problem. This pad presses up under the area that hurts to spread the metatarsal heads. It may be possible to build up the area using layers of duct tape rather than a pad, which may give more control over the shape and size of the pressure. However, if the problem is a stress fracture rather than a Morton's Neuroma, a metatarsal pad will aggravate the problem.
- Cortisone injections can help reduce the inflammation of the nerve, but often multiple injections are required and the relief may be temporary.
- Cortisone is a steroidal anti-inflammatory that may be able to break the vicious cycle of irritation and inflammation, and allow the nerve to heal. By temporarily shrinking the nerve, it is more likely to fit in between the metatarsals without irritation.
- There suggestions that cortisone can help in about 40% of cases and that relief can last for three months. Typically injections are given 1-3 weeks apart and should be given from the top of the foot or between the toes, not through the sole of the foot.
- Alcohol injections are generally considered a safe approach that can be effective.
- I could not find a clear explanation of the mechanism for the alcohol; but this technique is sometimes called "sclerosing" meaning to harden, or "neurolysis" meaning a temporary degeneration or blocking of the nerve.
- One study showed that 3 to 7 injections of a 4% alcohol solution every 5–10 days helped ~90% of cases. A ten month follow up indicated a reduction in the size of the neuroma.
- The injections combine alcohol with an anesthetic to reduce the pain. The treatment can leave is some residual, transient pain in some cases (~16%).
- Note that the alcohol injection should be guided accurately using ultrasound, which requires a skilled technician and this may limit the effectiveness of the treatment. Without the ultrasound guidance, the treatment does not seem as effective.
- If nothing else works, the nerve can be surgically removed, which is generally successful (~80%), though in some cases (~5%) the end of the removed nerve becomes inflamed and requires further surgery. If this approach is taken, it is recommended that the nerve is removed through the top of the foot to prevent scaring of the sole of the foot and reduce recovery times.
- There is little evidence to support the use of orthotics in treating Morton's Neuroma.
- Ice may help, but it does not seem as effective on this problem is it is on muscular problems.
- There are some recommendations for strengthening the muscles that flex the toes and support the arch of the foot, but I found no evidence to support this. Typical exercises would include scrunching up a towel with the toes, or picking up marbles with the toes.
5.1 Overnight Toe Spreading Sock
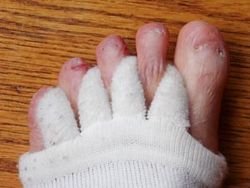
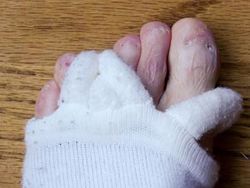
I found that using "Comfy Toes Foot Alignment Socks" has provided me with more relief than any of the other treatments I tried. A similar product is Happy Feet. These socks are intended to be used so that they stretch the gap between each toe, as shown below. I wore the socks like this overnight and found it helped quite a bit, but it did trigger quite a bit of pain as the toes were stretched in the night. (You can see the scar tissue on my feet from Epidermolysis Bullosa.)
I changed the usage so that all the stretch was between the toes that have the Morton's Neuroma, as shown below. This increased the stretch quite a bit and relieved the Morton's Neuroma further. It also reduced the pain I experienced overnight from the stretch.
There are plastic toe spreaders such as Pampered Toes, but I didn't find them as comfortable.
5.2 Shoe Modification
I routinely cut open the toe box of my shoes to allow my toes to spread while I run. This prevents blisters of the toes, and I believe it also increases my biomechanical efficiency. However, when I had a Morton's neuroma I cut far more of the shoe a way to prevent any pressure on the sides of my forefoot.
A friend did a rather more subtle change, opening up just the sides where the forefoot touches the shoe
- Category:Injury